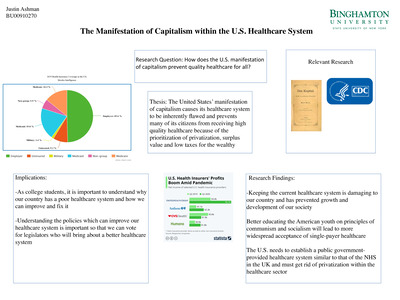
In conversations about healthcare systems worldwide, a recurring observation emerges: capitalist healthcare models often evoke a mix of admiration and critique. Many marvel at the innovation and advanced technologies fostered within these systems, yet simultaneously express frustration over accessibility and equity issues. This duality is not merely a surface-level contradiction but stems from deeper, systemic forces shaping the interplay between commerce and care. The truth about capitalist healthcare is complex, revealing insights about societal values, economic incentives, and the intricate balance between profit-driven motives and human well-being.
The Foundations of Capitalist Healthcare
Capitalist healthcare systems are fundamentally grounded in free-market principles, where private entities compete to deliver medical services and products. This model pivots on supply and demand, consumer choice, and entrepreneurial innovation. The premise is that market competition will spur efficiency and quality, incentivizing providers to offer superior care to attract and retain patients. Underneath this foundation lies an array of stakeholders—insurance companies, pharmaceutical firms, hospitals, and private practitioners—each operating within the confines of a profit-maximization ethos.
This architecture inherently prioritizes commodification of health services, turning medical care into a marketable good. The dynamic is that patients become consumers, and their health needs are subjected to market mechanisms. It is a paradigm that aligns well with capitalist ideals but simultaneously introduces tensions, as the intrinsic value of health challenges straightforward commodification.
Innovation and Technological Advancement
One of the frequently lauded attributes of capitalist healthcare systems is their capacity to drive innovation and rapid technological advancement. The profit motive often fuels significant investment in research and development, birthing breakthroughs in diagnostics, pharmaceuticals, and treatment methodologies. Competition among firms to patent new drugs or medical devices creates a fertile environment for scientific progress.
However, this inducement for innovation is a double-edged sword. While new technologies can drastically improve patient outcomes, they can also exacerbate inequalities. Cutting-edge treatments often come with exorbitant price tags, accessible primarily to wealthier demographics or through complex insurance schemes. Moreover, research prioritizes diseases and conditions that promise lucrative returns, potentially sidelining rare or less profitable ailments. This phenomenon reflects a selective innovation process shaped by market demand rather than purely medical necessity.
Access and Equity Challenges
Perhaps the most contentious aspect of capitalist healthcare is the disparity in access to essential services. When health is treated as a commodity, affordability becomes a barrier for many individuals, especially those without comprehensive insurance coverage or sufficient financial means. Costs for hospital stays, medications, and preventive care can spiral beyond the reach of large segments of the population, generating profound inequities.
The system’s response often involves intricate insurance networks and government interventions, but these solutions can add layers of complexity rather than clarity. Unlike universal healthcare models that strive for equitable access, capitalist systems emphasize individual responsibility for coverage. This approach can result in gaps that leave vulnerable groups exposed, highlighting a fundamental tension between market freedom and social welfare.
The Role of Insurance and Risk Management
Insurance companies play a pivotal role in capitalist healthcare, functioning as intermediaries between patients and providers. Their involvement introduces mechanisms of risk pooling and cost-sharing that aim to buffer the financial burden of illness. Yet, the insurance model is itself deeply embedded with profit objectives, influencing coverage decisions, premium pricing, and reimbursement policies.
This creates a landscape where health risk is not merely a medical concern but a commodity to be managed and underwritten. Insurance firms engage in practices such as risk selection and cost containment, which can lead to exclusionary tactics against high-risk individuals or chronic conditions. The resulting fragmentation can undermine continuity of care and exacerbate administrative overhead, making the system less patient-centric.
The Cultural Fascination with Capitalist Healthcare
The allure of capitalist healthcare is tied to broader cultural narratives valuing individualism, choice, and innovation. Many societies imbue the system with an aspirational mystique, equating market-led healthcare with progress and freedom. This fascination often masks less visible consequences by foregrounding success stories of cutting-edge treatments and medical entrepreneurship.
Additionally, capitalist healthcare intersects with deeply ingrained perceptions about self-reliance and meritocracy. The idea that one’s health outcomes correlate with personal effort and economic status resonates in capitalist cultures, reinforcing acceptance of inequalities. This narrative provides a psychological rationale that deflects critiques and sustains system legitimacy, even when disparities remain stark.
The Ethical Quandaries in Profit-Driven Care
At the heart of capitalist healthcare lie ethical dilemmas related to prioritizing profit over patient welfare. Healthcare providers and corporations face the persistent challenge of balancing fiduciary duties to shareholders against the Hippocratic imperative to care. This dynamic can engender conflicts of interest, where decisions about treatment modalities or resource allocation pivot more on financial calculus than medical necessity.
Critics argue that commodifying health distorts foundational ethical principles, reducing patients to revenue streams rather than human lives. Pricing strategies, marketing tactics, and corporate lobbying efforts further complicate the moral landscape, raising questions about justice, transparency, and accountability within the system.
The Impact on Public Health Outcomes
When evaluating capitalist healthcare’s efficacy, one cannot overlook its impact on population health metrics. The system’s strengths in innovation do not always translate into superior public health results. Countries with predominantly capitalist models sometimes report fragmented care, variable quality, and disparities in chronic disease management compared to systems with stronger public health infrastructures.
Preventive care and health promotion can be underemphasized because their benefits do not immediately generate profits. This short-term orientation potentially hinders long-term health improvements, as preventive interventions are often less lucrative than acute treatments. Consequently, capitalist healthcare may perpetuate a reactive rather than proactive approach to health, impeding broader societal well-being.
The Future Trajectory: Hybrid Models and Reforms
Recognizing the limitations inherent in pure capitalist healthcare systems, many nations are exploring hybrid models that blend market mechanisms with public oversight. These reforms seek to harness innovation and efficiency while expanding access and controlling costs. Examples include regulated insurance markets, government subsidies, and mandated coverage provisions.
The evolving landscape acknowledges that no singular approach can perfectly resolve the tensions between profit motives and equitable care. The future of healthcare likely lies in nuanced, context-sensitive frameworks that balance capitalist dynamism with strong ethical and social commitments. Such hybridization may offer pathways to reconcile the allure of capitalist healthcare with the imperative for universal human dignity in health.